PERIPHERAL NERVE DISEASES
by R.M. Clemmons, DVM, PhD
Associate Professor of Neurology & Neurosurgery
Introduction:
Dropped Jaw, muscle atrophy of the head, decreased facial sensation, inability
to close the eyelid or move the lip and ear, dysphagia, megaesophagus,
laryngeal paralysis and tongue paralysis are all signs associated with
specific cranial nerve abnormalities. Monoparesis or paralysis of one limb
or specific muscle group are signs of peripheral nerve dysfunction. The
cranial nerves are distinct from other peripheral nerves in a number of
ways. Generally, cranial nerves function in pairs with the sensory portion
of the reflex arc carried in one nerve and the motor portion of the arc
carried in another. Peripheral nerves are generally mixed nerves carrying
both motor and sensory information for the region, together. Cranial nerves
come from various branchial arches, while the peripheral nerves come form
the somites. As such the cranial nerves migrated with their organs to provide
the nervous innervation. In addition, each of the branchial arches has
a unique immunologic signature, while the peripheral nerves are very similar
immunologically. Each cranial nerve can be affected by selective immune
disorders, whereas immune disorders of the peripheral nervous system, generally,
affects all peripheral nerves.
The differential diagnosis for cranial and peripheral nerve disorders
includes trauma, inflammatory (or infectious), idiopathic (immunologic)
and neoplastic diseases. The facial nerve is susceptible to trauma at the
angle of the jaw. The radial nerve can be damaged by trauma as it passes
laterally along the humerus in the musculospiral groove. The sciatic nerve
can be damaged secondary to pelvic fractures. All cranial and peripheral
nerves can be affected by neoplasia including neurofibromas, neurofibrosarcomas,
schwannomas and lymphosarcoma. Immune attack against the neural-specific
proteins in cranial and peripheral nerves is not infrequent and leads to
either specific cranial neuropathies or polyradiculopathy.
Diagnostic Approach:
In peripheral nervous system diseases, the neurologic examination helps
to determine the location and extent of the disease process. Unless the
patient is too weak to support itself and move, there is no evidence of
long tract signs. The minimum data base includes a CBC, chemistry panel
and urinalysis. The former should include a measure of inflammation, such
as serum fibrinogen. The later is important to determine whether there
is immunologic effects within the glomeruli. Radiographs may help determine
the extent of trauma and location of osseous damage. Additional serum tests
for evidence of systemic or specific immunoreactivity may be helpful in
obtaining a diagnosis. In masseter and temporalis muscle atrophy, antibodies
against 2M antigens may confirm the diagnosis. The most important confirmatory
test is that of the EMG. The EMG can determine whether there is spontaneous
muscle potentials (fibrillation potentials and positive-sharp waves), whether
there are changes in motor or sensory nerve conduction velocities and whether
the is normal transmission across the neuromuscular junction. Muscle and
nerve biopsies may provide histopathologic diagnosis. Finally, exploratory
surgery may be indicated when localized lesions can be determined upon
neurologic or EMG examinations.
Specific Disorders
Diseases of Mastication:
 The trigeminal nerve
give rise to the sensory nerves for the skin and structures of the eye,
nose, mouth and face and the motor nerves to the muscles of mastication.
It consists of 3 major branches: the ophthalmic nerve which is sensory
to the structures of the orbit and skin of the dorsum of the nose; the
maxillary nerve which is sensory to the skin of the cheek, side of the
nose, muzzle, mucous membrane of the nasopharynx, maxillary sinus, soft
and hard palates and the teeth and gingivae of the upper jaw; and , the
mandibular nerve which is sensory to the remaining portions of the face
and mouth and is motor to the muscles of mastication. Diseases of the trigeminal
nerve or the muscles of mastication are not uncommon and must be differentiated
from one another.
The trigeminal nerve
give rise to the sensory nerves for the skin and structures of the eye,
nose, mouth and face and the motor nerves to the muscles of mastication.
It consists of 3 major branches: the ophthalmic nerve which is sensory
to the structures of the orbit and skin of the dorsum of the nose; the
maxillary nerve which is sensory to the skin of the cheek, side of the
nose, muzzle, mucous membrane of the nasopharynx, maxillary sinus, soft
and hard palates and the teeth and gingivae of the upper jaw; and , the
mandibular nerve which is sensory to the remaining portions of the face
and mouth and is motor to the muscles of mastication. Diseases of the trigeminal
nerve or the muscles of mastication are not uncommon and must be differentiated
from one another.
 Trigeminal neuritis
(an immune disorder affecting the myelinated pathways in the trigeminal
nerve) is usually transient, but can present as a significant problem.
The cardinal signs of trigeminal neuritis if a dropped jaw with the inability
to close the mouth. It affects adult dogs and cats with no breed or sex
predilection. It must be differentiated from fracture or subluxation of
the temporomandibular joint (evaluated by skull radiographs). On pathologic
examination, there is bilateral nonsuppurative neuritis of the trigeminal
nerve. As an idiopathic immune-related disorder, the condition will usually
improve over 1-3 weeks. On the other hand, methylprednisolone therapy may
help reduce the severity of an attack. Additional measures includes the
use of antioxidant medications such as vitamin E and C, n-acetylcysteine
and ginkgo biloba. These latter measures may help prevent reoccurrence
of episodes, which are occasionally seen. Other measures including feeding
liquified food and/or introduction of a PEG tubes to support nutrition
while the neuritis slowly responds. Some have supported the patients nutrition
by placing a wide rubber band around the mouth (which helps close the mouth)
while the patient is allowed to eat.
Trigeminal neuritis
(an immune disorder affecting the myelinated pathways in the trigeminal
nerve) is usually transient, but can present as a significant problem.
The cardinal signs of trigeminal neuritis if a dropped jaw with the inability
to close the mouth. It affects adult dogs and cats with no breed or sex
predilection. It must be differentiated from fracture or subluxation of
the temporomandibular joint (evaluated by skull radiographs). On pathologic
examination, there is bilateral nonsuppurative neuritis of the trigeminal
nerve. As an idiopathic immune-related disorder, the condition will usually
improve over 1-3 weeks. On the other hand, methylprednisolone therapy may
help reduce the severity of an attack. Additional measures includes the
use of antioxidant medications such as vitamin E and C, n-acetylcysteine
and ginkgo biloba. These latter measures may help prevent reoccurrence
of episodes, which are occasionally seen. Other measures including feeding
liquified food and/or introduction of a PEG tubes to support nutrition
while the neuritis slowly responds. Some have supported the patients nutrition
by placing a wide rubber band around the mouth (which helps close the mouth)
while the patient is allowed to eat.
Masseter and temporalis myositis is a chronic progressive disease which
presents with acute exacerbations and remissions. It is an auto-immune
disease directed at the unique antigenic markers of the muscles innervated
by the trigeminal nerve. The cardinal signs of this myositis is the inability
to open the jaw, which differentiates it from primary diseases of the trigeminal
nerve. In the acute phase, there is elevation of serum muscle enzymes (CPK,
AST, LDH and aldolase). On the CBC, there is often an elevation of eosinophils
(giving the condition its name, eosinophilic myositis). On the other hand,
in the chronic 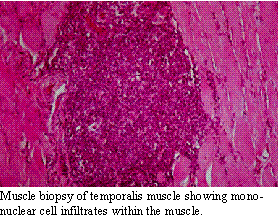 phase,
the amount of remaining muscle and, therefore, the amount of inflammation
are reduced. The diagnosis can be confirmed on muscle biopsy and determination
of serum antibody titers to the 2M antigen. The treatment of acute masseter-temporalis
myositis is with immunosuppressive medication. We use oral prednisolone
at 1 mg/kg/day divided into 2 or 3 doses for 1-2 weeks, followed by 0.5
mg/kg/day for 1-3 weeks. There is no evidence to suggest that keeping patients
on alternate day steroid therapy between attacks will reduce the chances
for progression. Here is another area where using dietary supplements might
be useful. In the chronic phase, the jaw may be locked shut. In these cases,
it may be necessary to manually open the mouth under anesthesia. This may
lead to fracture of the jaw. The hope is that, once the fibrosis is broken,
the remaining muscle mass will allow enough function for the patient to
be able to feed itself. The jaw must open about 1-1.5 inches for this to
happen.
phase,
the amount of remaining muscle and, therefore, the amount of inflammation
are reduced. The diagnosis can be confirmed on muscle biopsy and determination
of serum antibody titers to the 2M antigen. The treatment of acute masseter-temporalis
myositis is with immunosuppressive medication. We use oral prednisolone
at 1 mg/kg/day divided into 2 or 3 doses for 1-2 weeks, followed by 0.5
mg/kg/day for 1-3 weeks. There is no evidence to suggest that keeping patients
on alternate day steroid therapy between attacks will reduce the chances
for progression. Here is another area where using dietary supplements might
be useful. In the chronic phase, the jaw may be locked shut. In these cases,
it may be necessary to manually open the mouth under anesthesia. This may
lead to fracture of the jaw. The hope is that, once the fibrosis is broken,
the remaining muscle mass will allow enough function for the patient to
be able to feed itself. The jaw must open about 1-1.5 inches for this to
happen.
Facial Paralysis:
 The facial nerve
exits the brainstem in the cranial medulla and leaves the calivarium passing
near the inner ear (diseases here cause a number of facial nerve problems
which have already been discussed). It then travels cranially over the
ramus of the mandible to distribute to the muscles of facial expression.
Damage of the facial nerve results in decreased movement of the ear, eyelids
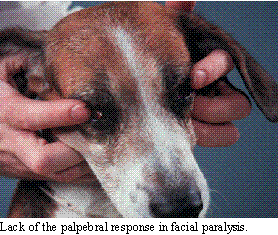
and buccal muscles. The menace response, palpebral reflex, lip reaction
and ear twitch response become decreased to absent. In evaluating the menace
response, it is necessary to determine that the animal is visual, either
by performing a dazzle response or evaluating the animal's visual behavior.
The palpebral reflex should be checked with the corneal reflex, indicating
that the problem is not sensory through the trigeminal nerve. The lip retraction
can be checked against response to placing a probe gently into the nares.
The ear response may be checked by observing the animal's head shaking
or pulling the head away. Remember to always check the tear production
with the Schirmer's tear test.
The facial nerve
exits the brainstem in the cranial medulla and leaves the calivarium passing
near the inner ear (diseases here cause a number of facial nerve problems
which have already been discussed). It then travels cranially over the
ramus of the mandible to distribute to the muscles of facial expression.
Damage of the facial nerve results in decreased movement of the ear, eyelids
and buccal muscles. The menace response, palpebral reflex, lip reaction
and ear twitch response become decreased to absent. In evaluating the menace
response, it is necessary to determine that the animal is visual, either
by performing a dazzle response or evaluating the animal's visual behavior.
The palpebral reflex should be checked with the corneal reflex, indicating
that the problem is not sensory through the trigeminal nerve. The lip retraction
can be checked against response to placing a probe gently into the nares.
The ear response may be checked by observing the animal's head shaking
or pulling the head away. Remember to always check the tear production
with the Schirmer's tear test.
Acute unilateral or bilateral facial nerve paralysis may be seen in
adult dogs, particularly in the cocker spaniel. There are no other signs
of neurologic disease. There is no evidence of otitis on physical, neurologic
or radiographic examination. EMG changes (fibrillation potentials and positive
sharp waves) are usually present in the muscle innervated by the facial
nerve, only. There is no therapy; but, if attention is given to supporting
tear production, the animal does not appear to have difficulty living with
its deficits. It is felt that this represents an autoimmune disease and
immune therapy may be indicated.
Polyneuropathy:
The most common polyneuropathy seen in dogs is acute polyradiculopathy.
This disorder is also referred to as "coonhound paralysis" since a great
number of hounds developed an ascending flaccid paralysis following contact
with raccoons. This suggests that there are a number of inciting causes
of polyradiculopathy in dogs, including something present in the bite of
the raccoon. Other patients experience similar syndromes following rabies
vaccination. It is probable that the inciting cause causes a cross-reactivity
with the neural antigens in the nerve roots, leading to demyelination and
the clinical signs.
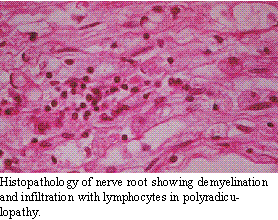 This disorder
can affect any age, breed or sex of dog or cat, although the condition
is rare before the age of 6 months. The onset of signs begins as rear leg
weakness which rapidly ascends over 24-48 hours until the animal is quadriplegic.
Occasionally, the condition can start in the fore legs and then progress
to quadriplegia. Physical examination is usually within normal limits (an
old raccoon bite might be apparent in hounds). Usually, there are no cranial
nerve signs; however, in severe cases, the bark may be altered, swallowing
impaired and facial nerve signs be evident. In some cases, respiration
is impaired necessitating respiratory support.
This disorder
can affect any age, breed or sex of dog or cat, although the condition
is rare before the age of 6 months. The onset of signs begins as rear leg
weakness which rapidly ascends over 24-48 hours until the animal is quadriplegic.
Occasionally, the condition can start in the fore legs and then progress
to quadriplegia. Physical examination is usually within normal limits (an
old raccoon bite might be apparent in hounds). Usually, there are no cranial
nerve signs; however, in severe cases, the bark may be altered, swallowing
impaired and facial nerve signs be evident. In some cases, respiration
is impaired necessitating respiratory support.
The diagnosis is supported by finding mild elevation of CSF protein,
particularly from lumbar spinal tap. The EMG reveals denervation potentials
(fibrillation potentials and positive sharp waves). The motor conduction
velocity is usually slower (< 50 M/sec), particularly later in the course
of the disease.
There is no specific treatment for polyradiculopathy. Corticosteroid
therapy may reduce the recovery time, but have not been shown to reduce
the time to reach maximal severity nor the eventual severity of the disease.
Recent evidence, support a role of antioxidant steroids (methylprednisolone)
in reducing clinical signs. When respiratory depression is evident, this
may be helpful in treating the patient. The clinical course is variable
and may last from a few days to several weeks. In some cases, there are
permanent neurologic deficits. Recovered animals may have the condition
reoccur. Recurrences are often more severe than the initial incident. Some
cases become chronic in nature, requiring more aggressive medication in
hopes of controlling the problem. I have found that many of these patients
respond better to antioxidant therapy with drugs like acetylcysteine or
ginkgo biloba than to steroid medication alone.
Brachial Plexus Injury:
A common neurologic injury from trauma (such as being hit by a car) is
that of brachial plexus avulsion. The brachial plexus is susceptible to
injuries that produce abduction of the thoracic limb from the body wall
or a direct blow to the lateral surface of the scapula. The cardinal signs
of brachial plexus avulsion are a monoplegia of one front leg, Horner's
syndrome on the affected side, lack of panniculus response on the side
of the lesion and a Babinski's sign in the ipsilateral rear leg. The nerve
roots are stretched or torn from their origin by this trauma, since the
meningeal coverings 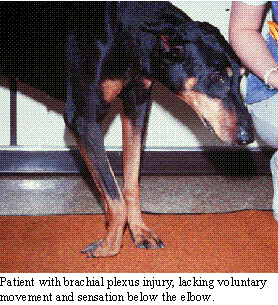 of
the nerve roots are thinner than those in the peripheral nerve. The epineurium
of the peripheral nerve is contiguous with the dural mater, providing extra
support to the peripheral nerves. In cases where the nerve roots have been
torn, recovery in unlikely without new experimental surgical techniques.
of
the nerve roots are thinner than those in the peripheral nerve. The epineurium
of the peripheral nerve is contiguous with the dural mater, providing extra
support to the peripheral nerves. In cases where the nerve roots have been
torn, recovery in unlikely without new experimental surgical techniques.
The diagnosis may be confirmed by EMG examination in 5-7 days. The evidence
of denervation will be evident. If there is no nerve conduction 72 hours
after the injury, then avulsion is most likely.
Treatment is with time, physical therapy and protection from injury.
If there is no problem with the leg, then amputation is not warranted until,
at least, 6 months of time has past. On the other hand, if the leg gets
infected or troubles the patient, amputation may help the patient. Serial
neurologic assessments and EMG examinations may help determine the ultimate
prognosis. Some patients experience "tingling" of the foot as healing occurs.
These patients can attack the foot causing considerable self-mutilation,
even months after the initial injury.
Copyright Dog2Doc.com 1997
All Rights Reserved
 Hop back to the Dog2Doc Home Page!
Hop back to the Dog2Doc Home Page!
Last updated 27 August 2002
 Trigeminal neuritis
(an immune disorder affecting the myelinated pathways in the trigeminal
nerve) is usually transient, but can present as a significant problem.
The cardinal signs of trigeminal neuritis if a dropped jaw with the inability
to close the mouth. It affects adult dogs and cats with no breed or sex
predilection. It must be differentiated from fracture or subluxation of
the temporomandibular joint (evaluated by skull radiographs). On pathologic
examination, there is bilateral nonsuppurative neuritis of the trigeminal
nerve. As an idiopathic immune-related disorder, the condition will usually
improve over 1-3 weeks. On the other hand, methylprednisolone therapy may
help reduce the severity of an attack. Additional measures includes the
use of antioxidant medications such as vitamin E and C, n-acetylcysteine
and ginkgo biloba. These latter measures may help prevent reoccurrence
of episodes, which are occasionally seen. Other measures including feeding
liquified food and/or introduction of a PEG tubes to support nutrition
while the neuritis slowly responds. Some have supported the patients nutrition
by placing a wide rubber band around the mouth (which helps close the mouth)
while the patient is allowed to eat.
Trigeminal neuritis
(an immune disorder affecting the myelinated pathways in the trigeminal
nerve) is usually transient, but can present as a significant problem.
The cardinal signs of trigeminal neuritis if a dropped jaw with the inability
to close the mouth. It affects adult dogs and cats with no breed or sex
predilection. It must be differentiated from fracture or subluxation of
the temporomandibular joint (evaluated by skull radiographs). On pathologic
examination, there is bilateral nonsuppurative neuritis of the trigeminal
nerve. As an idiopathic immune-related disorder, the condition will usually
improve over 1-3 weeks. On the other hand, methylprednisolone therapy may
help reduce the severity of an attack. Additional measures includes the
use of antioxidant medications such as vitamin E and C, n-acetylcysteine
and ginkgo biloba. These latter measures may help prevent reoccurrence
of episodes, which are occasionally seen. Other measures including feeding
liquified food and/or introduction of a PEG tubes to support nutrition
while the neuritis slowly responds. Some have supported the patients nutrition
by placing a wide rubber band around the mouth (which helps close the mouth)
while the patient is allowed to eat.
 The trigeminal nerve
give rise to the sensory nerves for the skin and structures of the eye,
nose, mouth and face and the motor nerves to the muscles of mastication.
It consists of 3 major branches: the ophthalmic nerve which is sensory
to the structures of the orbit and skin of the dorsum of the nose; the
maxillary nerve which is sensory to the skin of the cheek, side of the
nose, muzzle, mucous membrane of the nasopharynx, maxillary sinus, soft
and hard palates and the teeth and gingivae of the upper jaw; and , the
mandibular nerve which is sensory to the remaining portions of the face
and mouth and is motor to the muscles of mastication. Diseases of the trigeminal
nerve or the muscles of mastication are not uncommon and must be differentiated
from one another.
The trigeminal nerve
give rise to the sensory nerves for the skin and structures of the eye,
nose, mouth and face and the motor nerves to the muscles of mastication.
It consists of 3 major branches: the ophthalmic nerve which is sensory
to the structures of the orbit and skin of the dorsum of the nose; the
maxillary nerve which is sensory to the skin of the cheek, side of the
nose, muzzle, mucous membrane of the nasopharynx, maxillary sinus, soft
and hard palates and the teeth and gingivae of the upper jaw; and , the
mandibular nerve which is sensory to the remaining portions of the face
and mouth and is motor to the muscles of mastication. Diseases of the trigeminal
nerve or the muscles of mastication are not uncommon and must be differentiated
from one another.
 phase,
the amount of remaining muscle and, therefore, the amount of inflammation
are reduced. The diagnosis can be confirmed on muscle biopsy and determination
of serum antibody titers to the 2M antigen. The treatment of acute masseter-temporalis
myositis is with immunosuppressive medication. We use oral prednisolone
at 1 mg/kg/day divided into 2 or 3 doses for 1-2 weeks, followed by 0.5
mg/kg/day for 1-3 weeks. There is no evidence to suggest that keeping patients
on alternate day steroid therapy between attacks will reduce the chances
for progression. Here is another area where using dietary supplements might
be useful. In the chronic phase, the jaw may be locked shut. In these cases,
it may be necessary to manually open the mouth under anesthesia. This may
lead to fracture of the jaw. The hope is that, once the fibrosis is broken,
the remaining muscle mass will allow enough function for the patient to
be able to feed itself. The jaw must open about 1-1.5 inches for this to
happen.
phase,
the amount of remaining muscle and, therefore, the amount of inflammation
are reduced. The diagnosis can be confirmed on muscle biopsy and determination
of serum antibody titers to the 2M antigen. The treatment of acute masseter-temporalis
myositis is with immunosuppressive medication. We use oral prednisolone
at 1 mg/kg/day divided into 2 or 3 doses for 1-2 weeks, followed by 0.5
mg/kg/day for 1-3 weeks. There is no evidence to suggest that keeping patients
on alternate day steroid therapy between attacks will reduce the chances
for progression. Here is another area where using dietary supplements might
be useful. In the chronic phase, the jaw may be locked shut. In these cases,
it may be necessary to manually open the mouth under anesthesia. This may
lead to fracture of the jaw. The hope is that, once the fibrosis is broken,
the remaining muscle mass will allow enough function for the patient to
be able to feed itself. The jaw must open about 1-1.5 inches for this to
happen.
 The facial nerve
exits the brainstem in the cranial medulla and leaves the calivarium passing
near the inner ear (diseases here cause a number of facial nerve problems
which have already been discussed). It then travels cranially over the
ramus of the mandible to distribute to the muscles of facial expression.
Damage of the facial nerve results in decreased movement of the ear, eyelids
and buccal muscles. The menace response, palpebral reflex, lip reaction
and ear twitch response become decreased to absent. In evaluating the menace
response, it is necessary to determine that the animal is visual, either
by performing a dazzle response or evaluating the animal's visual behavior.
The palpebral reflex should be checked with the corneal reflex, indicating
that the problem is not sensory through the trigeminal nerve. The lip retraction
can be checked against response to placing a probe gently into the nares.
The ear response may be checked by observing the animal's head shaking
or pulling the head away. Remember to always check the tear production
with the Schirmer's tear test.
The facial nerve
exits the brainstem in the cranial medulla and leaves the calivarium passing
near the inner ear (diseases here cause a number of facial nerve problems
which have already been discussed). It then travels cranially over the
ramus of the mandible to distribute to the muscles of facial expression.
Damage of the facial nerve results in decreased movement of the ear, eyelids
and buccal muscles. The menace response, palpebral reflex, lip reaction
and ear twitch response become decreased to absent. In evaluating the menace
response, it is necessary to determine that the animal is visual, either
by performing a dazzle response or evaluating the animal's visual behavior.
The palpebral reflex should be checked with the corneal reflex, indicating
that the problem is not sensory through the trigeminal nerve. The lip retraction
can be checked against response to placing a probe gently into the nares.
The ear response may be checked by observing the animal's head shaking
or pulling the head away. Remember to always check the tear production
with the Schirmer's tear test.
 This disorder
can affect any age, breed or sex of dog or cat, although the condition
is rare before the age of 6 months. The onset of signs begins as rear leg
weakness which rapidly ascends over 24-48 hours until the animal is quadriplegic.
Occasionally, the condition can start in the fore legs and then progress
to quadriplegia. Physical examination is usually within normal limits (an
old raccoon bite might be apparent in hounds). Usually, there are no cranial
nerve signs; however, in severe cases, the bark may be altered, swallowing
impaired and facial nerve signs be evident. In some cases, respiration
is impaired necessitating respiratory support.
This disorder
can affect any age, breed or sex of dog or cat, although the condition
is rare before the age of 6 months. The onset of signs begins as rear leg
weakness which rapidly ascends over 24-48 hours until the animal is quadriplegic.
Occasionally, the condition can start in the fore legs and then progress
to quadriplegia. Physical examination is usually within normal limits (an
old raccoon bite might be apparent in hounds). Usually, there are no cranial
nerve signs; however, in severe cases, the bark may be altered, swallowing
impaired and facial nerve signs be evident. In some cases, respiration
is impaired necessitating respiratory support.
 of
the nerve roots are thinner than those in the peripheral nerve. The epineurium
of the peripheral nerve is contiguous with the dural mater, providing extra
support to the peripheral nerves. In cases where the nerve roots have been
torn, recovery in unlikely without new experimental surgical techniques.
of
the nerve roots are thinner than those in the peripheral nerve. The epineurium
of the peripheral nerve is contiguous with the dural mater, providing extra
support to the peripheral nerves. In cases where the nerve roots have been
torn, recovery in unlikely without new experimental surgical techniques.